Updates from September 2022 affecting the anesthesia industry that you don’t want to miss:
FDA Approves Anesthesia for Ocular Surface
Eyecare pharmaceutical company Harrow and anesthesia company Sintetica have developed an FDA-approved ocular surface anesthesia, Iheezo.
Doc Groups Ask Congress to Extend Payment Bonus for Alternative Payment Models
Without an extra incentive, provider groups won’t be able to change their practices, doctors and health policy experts said Thursday at a Capitol Hill briefing.
Physician Malpractice: 8 Stats to Know
Here are eight key statistics on physician malpractice, pulled from Medical Economics’ “2022 Physician Report,” WalletHub’s “2022 Best & Worst States for Doctors” and Medscape’s “2021 Physician Malpractice Report.”
7 Anesthesia Updates for ASC Leaders:
Here are seven anesthesia stories Becker’s has reported on since Sept. 1:
Moody’s Downgrades Envision, Citing High Bankruptcy Risk
Moody’s Investors Service cut Envision Healthcare’s credit rating to C, the lowest notch on its scale, reflecting a high probability of bankruptcy or a major restructuring at the physician staffing firm and ambulatory surgery center operator, the rating agency said.
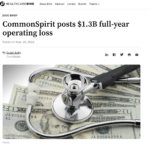
CommonSpirit Posts $1.3B Full-Year Operating Loss
CommonSpirit Health on Friday said higher expenses, especially for labor, and revenue challenges including an unfavorable shift in payer mix and declining acuity contributed to an operating loss of $1.3 billion in the fiscal year ended June 30. Last year, operating income was $998 million.
Stark Law Changes: Physician Compensation Arrangements to Keep an Eye On
Stay in the Know: Hospitals and health systems need to update their physician compensation plans after CMS’ recent changes to the Stark Law, according to an article in JDSupra from the law firm Foley and Lardner.
These arrangements should be “carefully reviewed” if the hospital seeks to meet the Stark Law employment or indirect compensation arrangement exceptions. Three things to note:
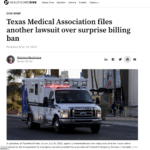
Texas Medical Association Files Another Lawsuit Over Surprise Billing Ban
Stay in the Know: The Texas Medical Association is suing the HHS over the final rule implementing a federal surprise billing ban, alleging the mechanisms for arbitrating payments unfairly favor insurers.
It's High Time for Broader Access to Non-Opioid Pain Medication
Limited Medicare coverage poses barriers, but bipartisan legislation offers a solution.
Physicians Brace for 8.42% cut to CMS Rates; Many Consider Dropping Medicare Patients
Physician practices are preparing for an 8.42 percent drop in Medicare payment rates next year because of the proposed 4.42 percent reduction in the CMS conversion factor and the 4 percent statutory Pay-As-You-Go sequester, which was implemented to offset congressional spending outside of healthcare.
ASA and APSF Update Guidance for Perioperative COVID-19 Screening
The American Society of Anesthesiologists and the Anesthesia Patient Safety Foundation (APSF) recently updated their recommended guidance for perioperative screening for SARS-CoV-2, the virus responsible for COVID-19.
The most important change regarding protocols for patients involves testing: “If community transmission is low or moderate, the patient is asymptomatic and without exposure, is vaccinated, and is undergoing a lower-risk procedure, healthcare systems could consider a more permissive approach to testing.”
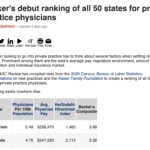
Becker's Debut Ranking of All 50 States for Private Practice Physicians
A physician looking to go into private practice has to think about several factors when settling on a location. Prominent among them are the area’s average pay, regulatory environment, amount of competition and individual insurance market.
Becker’s ASC Review has compiled data from the 2020 Census, Bureau of Labor Statistics, state regulations on new practices and the Kaiser Family Foundation to create a ranking of all 50 states for private practice physicians.
This ranking exists nowhere else.
Employed Physician Salary: 13 Stats
Medscape’s 2022 “Employed Physicians Report” surveyed more than 1,350 physicians employed by healthcare organizations, hospitals, large group practices, clinics or other medical groups about their jobs. Here are 13 stats about employed physician salary:
The No Surprises Act – Anticipating Unanticipated Consequences
A quick review of some of the more prominent features of the Act demonstrates why many providers and hospitals are concerned about serious consequences to the delicate contractual balance between insurers and healthcare providers.
Physician Burnout Higher in 2021 than 2020, Study Shows
Stay in the Know: About 63% of physicians surveyed experienced at least one manifestation of burnout in 2021, shooting up from 38% in 2020 and representing the highest amount in a decade of recurring survey findings, according to an article published this week in Mayo Clinic Proceedings.
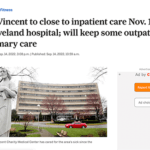
St. Vincent to Close to Inpatient Care Nov. 15 at Cleveland Hospital; Will Keep Some Outpatient, Primary Care
Stay in the Know: St. Vincent Charity Medical Center, which has been caring for Cleveland’s sick since the Civil War era, announced Wednesday that in mid-November it will stop offering inpatient, surgical and emergency room care.
ACOs Fight Looming Cuts, Privatization Rhetoric
Stay in the Know: Without congressional action, 5% bonus for advanced alternative payment models disappears in 2023
Beaumont-Spectrum to cut 400 jobs amid ‘significant’ financial pressure
Stay in the Know: Beaumont Health and Spectrum Health, now BHSH System, plan to cut 400 jobs as the Michigan health system faces “significant financial pressures,” the system told Healthcare Dive.
5 Thoughts on the Downside to Physician Employment
Stay in the Know: In its 2022 “Employed Physicians Report,” Medscape surveyed more than 1,350 physicians employed by healthcare organizations, hospitals, large group practices, clinics or other medical groups about their jobs.
Here are five quotes from anonymous employed physicians about the downsides of their jobs:
Anesthesiology Residency Programs with the Most Openings
Stay in the Know: According to a report from the American Medical Association, there are around 1,774 open first-year positions for anesthesiology residents. The University of Miami tops the list with the most openings for residents.
Ten anesthesiology residency programs with the most open positions-
Death of Anesthesiologist who Worked at Temporarily Closed Texas ASC Under Investigation
Anesthesiologist Melanie Kaspar, MD died on June 21. She was originally thought to have had a heart attack, but the Dallas County Medical Examiner ruled her death to be from the effects of the local anesthetic bupivacaine. The surgery center also temporarily paused operations following a medical emergency involving an 18-year–old boy in which a “compromised” IV bag was found at the facility.
The Types Of Anesthesia Explained
Under the two main categories of anesthesia, the American Society of Anesthesiologists (ASA) explains there are three types of analgesic anesthesia: local, regional, and general. Here are the types of anesthesia explained:
Steps for Reducing Environmental and Financial OR Waste
A quality improvement project at the University of California San Francisco not only identified obstacles to reducing such waste, but provided clinicians with concrete steps they could take to address these shortcomings.
Current insurer calculation of qualified payment amount for out-of-network OON care may violate No Surprises Act: American Society of Anesthesiologists
In possible violation of the No Surprises Act, health insurance company calculations of Qualified Payment Amounts (QPA) for anesthesiology, emergency medicine and radiology services (and possibly other specialty services) likely include rates from primary care provider (PCP) contracts. A new study conducted by Avalere Health and commissioned by three national physician organizations examined a subpopulation of PCPs and determined that contracting practices may directly impact the QPA.